
Estimated reading time: 6 minutes
504 accommodations for OCD are school supports specifically designed to reduce disruption from obsessions and compulsions without reinforcing OCD behaviors. That means limiting reassurance, avoiding repeated checking or rewriting, and supporting your child in tolerating uncertainty while staying engaged in schoolwork.
If your child is rewriting assignments, asking constant “what if” questions, or melting down when things don’t feel “just right,” that’s OCD—not defiance. Many traditional supports can accidentally feed the OCD loop, so a 504 plan for OCD has to be built differently.
This guide shows you how to get effective 504 accommodations for OCD and advocate for support that truly helps your child.

What are 504 accommodations for OCD?
A 504 accommodations plan for OCD is a school-based support plan that helps students manage intrusive thoughts, compulsions, and anxiety loops so they can access learning.
These supports fall under Section 504 of the Rehabilitation Act, which ensures students with medical or mental health conditions receive equal access to education.
👉 But here’s the key:
OCD accommodations are not about making things easier—they’re about helping kids function without strengthening compulsions.
Story time:
I had the opportunity to work with a lovely student once. Her name was Marley. Marley was able to hide her OCD for a long time until the writing demands of high school uncovered her writing rituals and perfectionism. Coupled with treatment in our BrainBehaviorReset ™ Program, Marley benefited from a 504 Plan with accommodations for writing. Instead of giving her extra time, which fed into her OCD, her teacher asked her to turn her work in with no revisions. She actually got downgraded if she made revisions.
These exposures were done with support from our OCD specialist and the school team to help Marley cope with her intrusive thoughts. Over time, with neurofeedback, PEMF and OCD ERP therapy, Marely was able to completely extinguish her OCD.
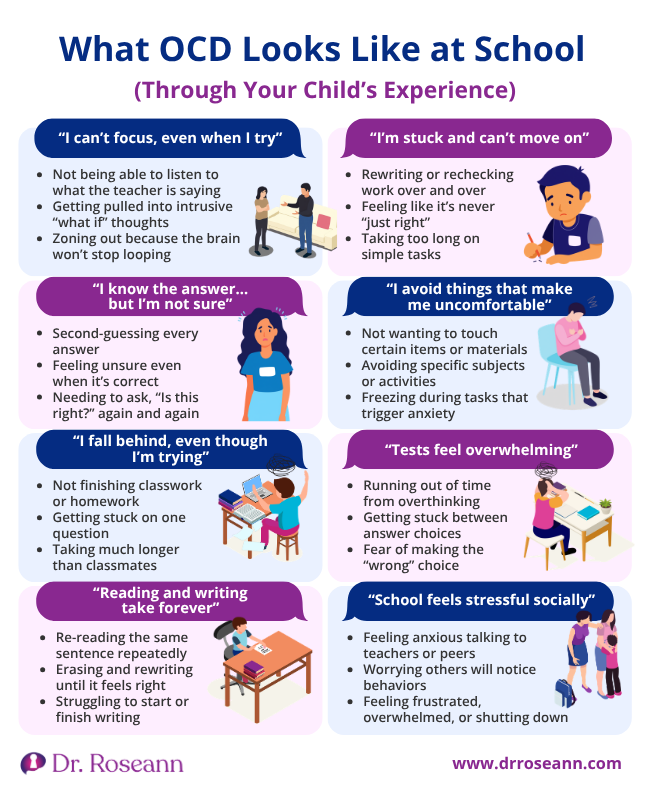
How does OCD show up at school?
There are a lot of myths about OCD but OCD is all about avoiding that totally irrational “bad thing” from happening when you don’t complete a mental ritual or behavior.
Research shows that OCD symptoms often wax and wane with life stress, (Kalanthroff et al., 2025) which is why your child may seem “fine” one week and really struggle the next. Underneath it all is an overactive brain loop—what scientists call the cortico-striatal-thalamo-cortical (CSTC) circuit—which keeps thoughts and urges stuck on repeat and can be incredibly mentally exhausting (Shephard et al., 2021).
Additionally, OCD doesn’t always look obvious. Many kids are quietly struggling in ways that teachers may misinterpret.
Common school struggles with OCD:
- Getting stuck rewriting or erasing work repeatedly
- Taking excessive time due to “just right” feelings
- Avoiding assignments that trigger intrusive thoughts
- Asking for repeated reassurance: “Is this okay?”
- Mentally checking, counting, or repeating silently
- Difficulty transitioning between tasks
Parent example:
Sophie, age 10, spent 30 minutes writing one sentence because it didn’t “feel right.”
Her teacher thought she was being perfectionistic—but she was actually stuck in a compulsive loop.
👉 Once her school understood this, they shifted expectations—and everything changed.
Takeaway: Behavior is communication. OCD often hides behind “good student” behavior.
How do I know if my child qualifies for a 504 plan?
If OCD is interfering with your child’s ability to function at school, they likely qualify.
Signs your child may need a 504 plan for OCD:
- Work takes significantly longer due to compulsions
- They experience distress during assignments or tests
- OCD leads to avoidance or shutdowns
- They need support to complete tasks or transitions
👉 The key question schools ask:
Does OCD limit your child’s access to learning?
If yes—you have a strong case.
What accommodations actually help OCD (without reinforcing it)?
This is where most resources get it wrong.
Helpful OCD school accommodations focus on:
👉 reducing distress
👉 supporting regulation
👉 NOT feeding compulsions

Effective 504 accommodations for OCD:
- Extended time with limits (to prevent endless rechecking)
- “Good enough” work expectations
- Reduced workload during flare-ups
- Structured check-ins instead of constant reassurance
- Breaks to reset when stuck in compulsions
- Clear “done” signals from teachers
- Support transitioning away from stuck behaviors
Regulation-first supports:
- Calm-down space for intrusive thought spikes
- Visual reminders: “Done is better than perfect”
- Predictable routines to reduce uncertainty
.png)
What accommodations can make OCD worse?
This is the most important—and most overlooked—part.
Some accommodations may feel helpful but actually strengthen OCD patterns.
Bad vs Good Accommodations for OCD
👉 Why this matters:
OCD grows through:
- avoidance
- reassurance
- repetition
So we support the child—but not the OCD cycle.
Expert insight:
“The goal of treatment is not certainty, but learning to tolerate uncertainty.” — Dr. Jonathan Abramowitz
How to get a 504 plan for OCD?
Here’s a simple path to follow:
Step-by-step:
- Submit a written request for evaluation
- Provide documentation (diagnosis, therapist notes)
- Attend the 504 meeting
- Collaborate on OCD-specific accommodations
- Monitor and adjust regularly
How to advocate for OCD-specific support at school?
Advocacy is where real change happens.
Use specific language:
Instead of:
❌ “My child has anxiety”
Say:
✔️ “My child has OCD with intrusive thoughts and compulsions that interfere with task completion”
Ask for:
- ERP-informed accommodations
- Teacher training on OCD patterns
- A consistent response plan (no reassurance loops)
Final Thoughts
If your child is struggling with OCD at school, I want you to hear this:
You’re not alone—and it’s gonna be OK.
Understanding OCD as a brain-based loop—not a behavior problem—changes everything. And advocating for the right 504 accommodations for OCD is one powerful step in helping your child succeed.
Because when we calm the brain first, everything becomes more possible.
Frequently Asked Questions
What are 504 accommodations for OCD?
504 accommodations for OCD are school supports that help your child manage intrusive thoughts and compulsions so they can stay engaged in learning without getting stuck.
Can 504 accommodations for OCD make symptoms worse?
Yes, 504 accommodations for OCD can make symptoms worse if they allow reassurance-seeking, avoidance, or compulsions, so they need to support regulation—not reinforce OCD.
What are examples of OCD school accommodations in a 504 plan?
Examples of OCD school accommodations include time limits on tasks, reduced workload, structured check-ins, and gentle teacher prompts to help your child move past compulsive behaviors.
Does my child need an OCD diagnosis to get a 504 plan?
Your child doesn’t always need an OCD diagnosis to get a 504 plan, but having documentation of OCD can make it easier to secure the right accommodations.
Is ERP therapy included in a 504 plan for OCD?
ERP therapy isn’t typically written into a 504 plan, but a 504 plan for OCD can include supports that align with ERP strategies, like limiting reassurance and encouraging gradual exposure.
How do I ask my child’s school for 504 accommodations for OCD?
To ask for 504 accommodations for OCD, you can submit a written request to your school and share how OCD symptoms are impacting your child’s learning and daily functioning.
What’s the difference between a 504 plan and an IEP for a child with OCD?
A 504 plan for OCD provides accommodations to access learning, while an IEP includes specialized instruction—most kids with OCD start with a 504 unless learning is significantly impacted.
How often should a 504 plan for OCD be reviewed or updated?
A 504 plan for OCD should be reviewed at least once a year, but you can request updates anytime your child’s OCD symptoms or needs change.
What should I do if my child’s 504 accommodations for OCD aren’t working?
If your child’s 504 accommodations for OCD aren’t working, you can call a meeting to adjust the plan so it better supports regulation and doesn’t unintentionally reinforce OCD behaviors.
Citations
Kalanthroff, E., Berebbi, S., David, M., & Simpson, H. B. (2025). Acute trauma and obsessive compulsive disorder: Evidence from October 7th, 2023. Psychotherapy and Psychosomatics. Advance online publication. https://doi.org/10.1159/000548026
Shephard, E., Stern, E. R., van den Heuvel, O. A., Costa, D. L., Batistuzzo, M. C., Godoy, P. B. G., Lopes, A. C., Cappi, C., Shavitt, R. G., Simpson, H. B., Miguel, E. C., & do Rosário, M. C. (2022). Neurocircuit models of obsessive-compulsive disorder: Limitations and future directions for research. Brazilian Journal of Psychiatry, 44(2), 190–203. https://doi.org/10.47626/1516-4446-2020-1231
Wu, M. S., McGuire, J. F., Martino, C., Phares, V., Selles, R. R., & Storch, E. A. (2016). A meta-analysis of family accommodation and OCD symptom severity. Clinical Psychology Review, 45, 34–44. https://doi.org/10.1016/j.cpr.2016.03.003
Always remember… “Calm Brain, Happy Family™”
Disclaimer: This article is not intended to give health advice and it is recommended to consult with a physician before beginning any new wellness regime. The effectiveness of diagnosis and treatment vary by patient and condition. Dr. Roseann Capanna-Hodge, LLC does not guarantee certain results.
Are you looking for SOLUTIONS for your struggling child or teen?
Dr. Roseann and her team are all about solutions, so you are in the right place!
.png)

%20.png)















